You're a Match: A Donor's Online Guide to Donation
Help for every step in the donation process
Why you have been asked to donate
You have been identified as a possible donor for a patient who seeks a marrow or peripheral blood stem cell (PBSC) transplant. When you joined the NMDP Registry, you agreed to consider donating cells from your marrow or blood to possibly help any patient in the world who may benefit from a transplant. You gave a blood or tissue sample when you joined. That sample was tested to determine your tissue type, and the test results were listed on the NMDP Registry

Now, a doctor searching the registry has identified you as a possible match for a patient who seeks a transplant.
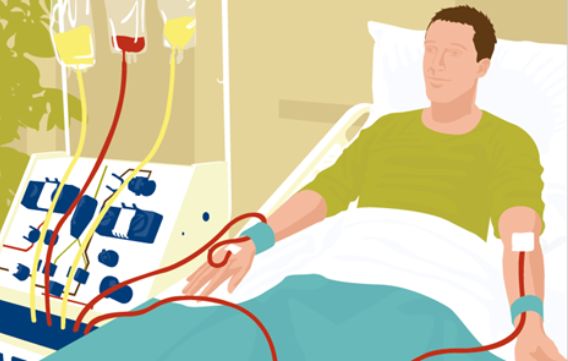
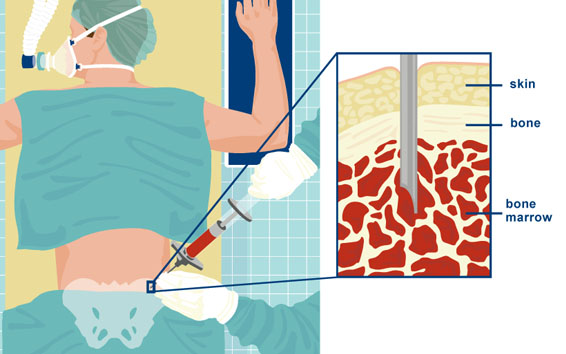
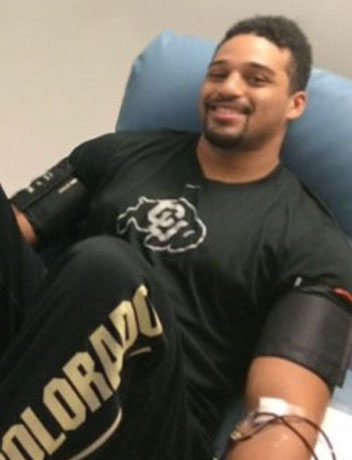
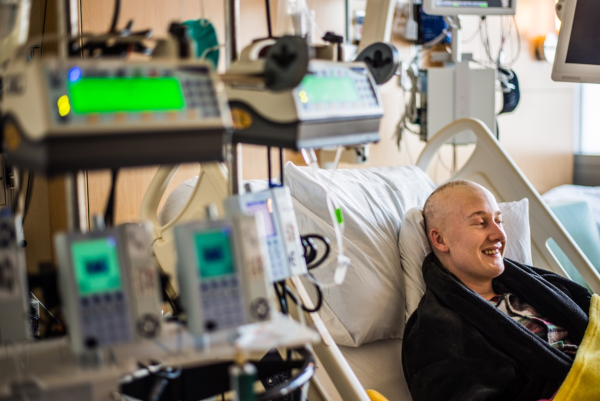
If you agree to donate, blood-forming cells collected from your marrow or bloodstream (which are PBSCs) will be transplanted into the patient to replace his or her marrow. A marrow or PBSC transplant can often help patients with leukemia, lymphoma, sickle cell disease and other life-threatening diseases live longer, healthier lives.
A transplant requires carefully matching the tissue type of the donor and the patient. Because tissue type is inherited, a patient’s brother or sister usually has the best chance of matching. If a match cannot be found within the patient’s family, the search is started to find an unrelated donor, like you. For more information about becoming a donor, reference pages 9-19 of the donor work up book.
- Complete a Health History Screening Questionnaire: page 10
- Learn more about the process: pages 12-19
- Make an informed decision about donating: pages 10-11
Step up to save a life
When you joined the NMDP Registry®, NMDP Program®, you learned that one day you might be called to donate to a patient who could benefit from a transplant.
We deeply appreciate the time and effort you have already given to NMDP, and thank you for considering becoming a marrow or peripheral blood stem cell, PBSC, donor.
Becoming a donor is a serious commitment. It’s important to understand what’s involved, so you can make an informed decision about whether or not you will donate. Visit the tabs above to learn more or download the full You’re a Match: A Donor’s Online Guide to Donation.
Your donor center representative will also work with you to answer your questions, but you will be the one to make the final decision about donating. You may agree to more testing to get ready to donate, or you can say you prefer not to donate at this time.
Thank you again for the time and effort you have already given to NMDP and for considering becoming a donor.
Our Guide to Donation is available in the following languages: Spanish, Portuguese, Korean, Vietnamese, and Chinese.